Comedonal Acne Guide: Causes, Treatments, And Prevention
Popping is not the solution, especially when you have more appropriate treatment options.

Image: i Stock
Comedonal acne is a mild form of acne. Comedones are blocked pores that later develop into pimples and more severe forms of acne. Blackheads and whiteheads are the most common examples of comedonal acne.
They are not as inflammatory or painful as other severe forms of acne. However, you still need to follow self-care practices and use topical or oral medications to manage them. Read on to learn more about them and ways to minimize them.
In This Article
What Is Comedonal Acne?
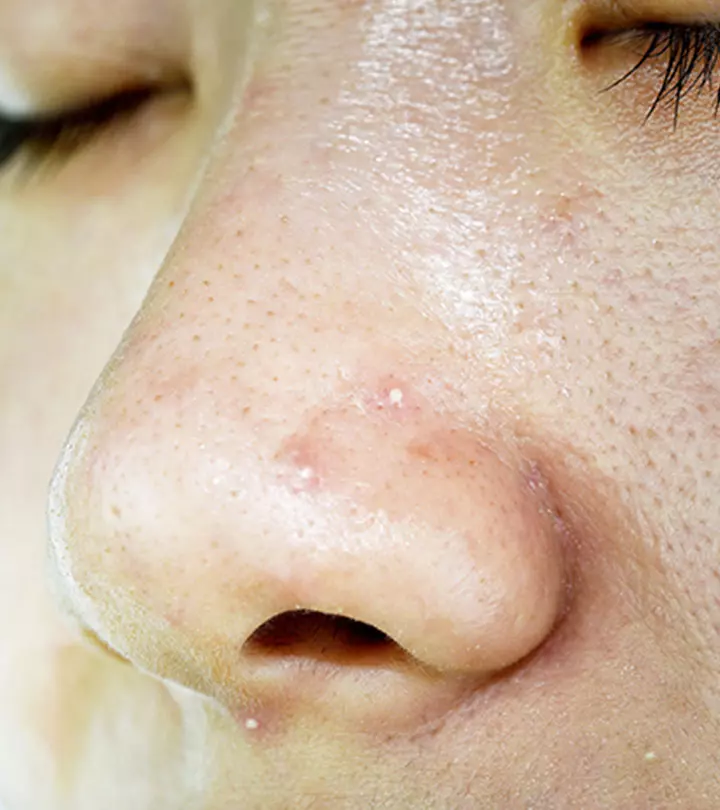
Comedonal acne is a type of acne that appears like comedones (blocked pores that mostly occur on the nose, chin, and forehead). The pores are plugged due to excessive sebum production, oil, dirt, and dead skin cells. Blackheads and whiteheads are the most common types of comedonal acne. When the dirt and oil plugs are exposed to air, they oxidize and turn black, resulting in blackheads. When these plugs are set deeper into the pores and are white, you get whiteheads.
In a study conducted on 44,689 participants from 27 countries, it was found that 43.35% of them had one dermatological condition last year, of which 12% had acne. Further, the overall prevalence of acne was 5.4%, and it was reported as one of the most common skin conditions in people over 18 years. A comedonal acne is a mild form of acne that you can manage by using home remedies.
In the following section, we will look at the causes and risk factors of comedonal acne.
Key Takeaways
- Comedonal acne is commonly prevalent as blackheads and whiteheads.
- They are filled with oil, dirt, and dead skin cells and are less inflammatory and painful.
- Topical treatment, oral medications, and surgical procedures can be advised by the doctor for treating them.
- Make sure you use non-comedogenic products for skincare and makeup and wash your face twice daily with a gentle cleanser.
Comedonal Acne: Causes And Risk Factors

Comedonal acne is caused when the sebaceous ducts are blocked with dirt, debris, and sebum. While anyone can get comedonal acne at any point in time, certain factors increase the risk:
- Dairy (such as yogurt, milk, and cheese) consumption may cause acne (1).
- Diet with a high glycemic index/glycemic load may aggravate acne (2). Consuming foods that contain a lot of sugar and fat (such as baked goodies, junk food, and aerated drinks) may cause breakouts.
- Some believe excessive water intake may also cause acne. Your skin may get overhydrated due to humid conditions or from excessive use of moisturizers.
- Smoking may also cause acne and breakouts (3).
- Using excessive makeup, oily skincare products, and hair pomades may cause acne.
- Genetics may also be a factor behind comedonal acne. If it runs in your family, you are most likely to get it.
- Squeezing the existing comedones and excess use of abrasive skin products for exfoliation (such as scrubs and chemical exfoliants) may also aggravate your condition and cause comedonal acne.
Apart from blackheads (open comedones) and whiteheads (closed comedones), there are several other types of comedones.
Types Of Comedonal Acne
1. Microcomedones
These are the smallest comedones. They are invisible to the naked eye. They are the first stage of every blackhead, inflamed acne, or pimple.
2. Macrocomedones
These can be both open and closed comedones, but they are larger.
3. Giant Comedones
Giant comedones are large blackheads, with a diameter measuring between a few millimeters to about 2 centimeters. Older adults usually get this type of comedones.
4. Solar Comedones
These are also called senile comedones and are caused by excessive sun exposure. These can be open or closed type comedones and can be large or small. These are common in older adults.
It is very easy to identify comedones once we know what they look like.
How To Identify Comedonal Acne

Here are a few tips to identify comedones:
- They look like black or white dots on the skin. The affected area feels uneven and bumpy.
- Blackheads will have a tip that appears dark brown or black. You will commonly see them on your nose.
- Whiteheads look like small whitish dots on your skin.
If you have comedonal acne, there is nothing to worry about. If you are struggling with how to get rid of whiteheads or blackheads, there are plenty of treatment options to manage them. In the next section, we have discussed these in detail.
How To Treat Comedonal Acne
1. Topical Treatment
Topical treatments are readily available as OTC medicines. However, you need to know the right percentage of the ingredients that will work for your condition. Consult a doctor before trying out any topical treatment. These are available in the form of gels, creams, and face washes. The most common ingredients used for treating comedonal acne are:
- Benzoyl Peroxide (4)
- Azelaic Acid (5)
- Salicylic acid (6)
- Sulfur (7)
- Tretinoin (or Retinoids) (8)
- Alpha-hydroxy acids (AHAs) (9)
- Beta-hydroxy acids (BHAs) (9)
Stronger retinoids need to be prescribed by a doctor. This is because using the wrong percentage of retinoids may cause irritation to the skin.
A beauty blogger, shared her personal experience of using salicylic acid to prevent her comedonal acne. She said, “This is hands-down one of the most sought-after ingredients by me. I have been using Salicylic Acid for as long as I could remember (i).”
2. Oral Medications

Topical medicines are good for initial acne treatment. However, depending on your needs, the doctor may also prescribe you oral medications such as:
- Accutane or Isotretinoin (mainly used for severe acne) (10)
- Contraceptives or birth control pills (FDA has approved only three contraceptives for acne, so ensure you do not take them without a doctor’s prescription) (10)
- Antibiotics (for comedonal acne turning in to inflammatory acne )
- Spironolactone (mainly formulated for hypertensioni A condition affecting the arteries where blood pressure is higher than normal. ; but this medicine, in low doses, may help hormonal acne as it blocks androgeni A sex hormone that characterizes the development of sexual characteristics in males. ) (10)
3. Surgical Procedures
Many wonder when does acne stop? The answer varies, but if both topical and oral medications fail to deliver results, you may opt for surgical procedures. Some of these procedures include:
- ComedoneExtraction: Comedones are removed manually by the doctor with an instrument called comedone extractor.
- Microdermabrasion: In this process, a device with a crystal head is rubbed on your skin to remove the top layer of your skin. This helps remove the comedones.
- Electrosurgery: This is used for treating severe comedonal acne. In this procedure, electricity is used to destroy the tissue by dehydration, coagulation, or vaporization. There are two types of electrosurgery – high-frequency electrosurgery and electrocauteryi A procedure that uses electric current to destroy abnormal tissue (such as lesions or tumors) or to stop bleeding after surgery. .
Microneedling and laser therapy may also help eliminate comedones and are less invasive than most dermatology treatments. However, consult a dermatologist to know the risks of these treatments before trying them.
4. Home Remedies
You may also take care of comedones at home by trying a few home remedies using simple and effective ingredients:
1. Tea Tree Oil
Five percent topical tea tree oil was found to be effective in treating mild to moderate acne (11).
You Will Need
- 2-3 drops of tea tree oil
- 1 teaspoon of any carrier oil (you may use jojoba, olive, sweet almond oils)
Method
- Mix the oils.
- Massage the mixture on the affected area.
- Leave it on for at least 20-30 minutes.
- Wash off.
How Often
Once daily or on alternate days.
 Quick Tip
Quick Tip2. Witch Hazel

Witch hazel is commonly used for relieving inflammation and skin irritation(12). Though there is a lack of direct evidence, anecdotal evidence suggests that it has an astringent effect and can help minimize acne.
You Will Need
- A tablespoon of witch hazel
- Cotton pad
Method
- Wash your face and pat it dry.
- Saturate the cotton pad with witch hazel.
- Apply it as a toner to your skin.
- Let it dry.
- Follow it up with a non-comedogenici Any cosmetic ingredient or skin care product that does not clog pores. moisturizer.
How Often
Once every day or on alternate days (do not overuse as it may dry your skin out).
3. Charcoal And Clay Mask
Activated charcoal works as an absorbent (13). It can eliminate dirt and sebumi An oily, waxy substance produced by the sebaceous glands that keep skin moist and prevent drying. from your skin. The clay (especially bentonite clay) can soothe the skin and heal skin lesions (14).
You Will Need
- ½ teaspoon of activated charcoal powder
- 2 tablespoons of bentonite clay
- Water for mixing (you may use rosewater)
Method
- Mix the charcoal powder and the clay.
- Add water or rosewater as per the desired consistency and mix well.
- Spread the mixture on the affected area.
- Let it dry.
- Wash off with warm water.
- Follow up with a non-comedogenic moisturizer.
How Often
Not more than 2 times a week.
4. Apple Cider Vinegar
Though there is no direct evidence, anecdotal evidence suggests that the vinegar may work well as a toner.
It also may act as an astringent and minimize skin pores, thus helping relieve acne. However, never use ACV without diluting it.
You Will Need
- ½ teaspoon of apple cider vinegar
- 2 tablespoons of distilled water (to dilute the ACV)
- Cotton pad
Method
- Wash your face and pat it dry.
- Mix the ACV and distilled water.
- Saturate the cotton pad with the mixture and apply it to your face as a toner.
- Let it dry and then apply a non-comedogenic moisturizer.
5. Oregano Oil
Oregano oil has antimicrobial and anti-inflammatory properties. It contains carvacrol, a natural compound with powerful antibacterial abilities, making it effective against the bacteria that can cause acne. Additionally, its anti-inflammatory properties may help reduce redness and swelling associated with acne (1).
You Will Need
- 1-2 drops of pure oregano essential oil
- 1-2 teaspoons of carrier oil (coconut oil or jojoba oil)
Method
- Mix oregano essential oil with carrier oil to dilute it.
- Apply the diluted oregano oil directly onto the affected acne spots with a clean cotton swab.
- Let it sit for a couple of hours or overnight.
- Rinse it off gently with lukewarm water.
- Apply a gentle, non-comedogenic moisturizer afterward.
How Often
Once a day
In addition to these treatment options, modifying your lifestyle also helps. In the following section, we have discussed the measures you can take to prevent comedonal acne.
Ways To Prevent Comedonal Acne

1. Wash Your Face Twice A Day
Use a mild cleanser or face wash containing salicylic acid to wash your face two times a day.
2. Use Non-comedogenic Products
Whether it is makeup or skincare, ensure you use non-comedogenic and oil-free products. This way, your skin pores won’t get clogged, and you can prevent comedonal acne.
3. Remove Makeup Before Going To Bed
Removing makeup before hitting the bed allows your skin to breathe and heal itself while you sleep.
4. Keep Your Skin Accessories Clean
Clean your makeup applicators, brushes, and beauty blenders thoroughly after every use. Dirty accessories may accumulate bacteria and aggravate acne-prone skin.
5. Follow A Healthy Diet
Following a daily skincare routine and a healthy lifestyle can help keep your skin clear to an extent. However, you may face breakouts from time to time, and you need to treat them properly. The methods outlined in this article can help. In case you have severe acne, it is always better to consult a doctor.
Reduce the intake of fried or processed foods, baked goodies, and sugary drinks. If possible, try to limit your milk intake. Instead, consume a lot of fresh vegetables and fruits that are rich in nutrients like vitamin C, vitamin E, and zinc. Also, consume lean protein.
6. Stay Hydrated
Drinking plenty of water keeps your body hydrated and makes your skin look healthier (16). When you are well-hydrated, your skin functions better, reducing the likelihood of clogged pores and breakouts.
7. Stay Active
Regular exercise boosts blood flow to the skin, raises skin temperature, and enhances skin moisture, which may benefit your skin (17). Sweating during exercise may also help purge toxins from your pores, but remember to cleanse your skin afterward to prevent buildup.
8. Manage Stress
High stress can trigger breakouts (18). So try meditation, deep breathing, or hobbies to keep stress levels low. Reducing stress helps regulate the hormones that contribute to acne, giving your skin a chance to heal and stay clear.
 Quick Tip
Quick TipInfographic: Dos And Don’ts Of Treating Comedonal Acne
Comedonal acne is characterized by flesh-colored bumps that develop due to genetics, excessive use of makeup, and poor lifestyle habits. However, proper treatment and a healthy lifestyle can help you manage them effectively. We have listed some simple tips you may benefit from while treating comedonal acne. Check out the infographic below to know more.
Some thing wrong with infographic shortcode. please verify shortcode syntaxComedonal acne is different from inflammatory acne and is caused by clogged pores, giving your skin a rough and bumpy appearance. While it is not a severe form of acne, the comedones may turn into inflammatory lesions if ignored. Therefore, following a regular skin care routine that includes anti-acne ingredients and products is crucial. You may use the remedies suggested in the article to soothe your skin and follow the tips to maintain a healthy lifestyle. and stress management. However, consult a doctor to determine the best medical treatment method for your condition.
Frequently Asked Questions
Does Accutane help treat comedonal acne?
Yes, it works for severe acne. Accutane is a form of vitamin A that reduces the amount of oil released by the skin’s oil glands. However, you shouldn’t take it without consulting your doctor.
Do closed comedones heal?
They can heal with proper treatment. However, if left untreated, they may turn into a serious issue.
Is comedonal acne hormonal?
Comedonal acne is mainly caused during the pre-teen years and is regulated by hormones. However, one may even experience them at a later point of their lives. Apart from hormonal changes, another major cause of this type of acne is poor skin hygiene. Certain products (shampoos, makeup, hair pomades) may also lead to comedonal acne as these contain chemicals and oils that may block the pores.
Is comedonal acne fungal?
No, there is a difference between fungal acne and comedonal acne. Fungal acne is caused by a yeast called Malassezia that causes an infection in the hair follicles whereas comedonal acne is a non-inflammatory acne caused by blocked pores.
Is comedonal acne itchy?
Comedonal acne may involve less level of itching in comparison to other types of acne.
Illustration: Comedonal Acne: Causes, How To Treat It, & Ways To Prevent It

Image: Stable Diffusion/StyleCraze Design Team
References
Articles on StyleCraze are backed by verified information from peer-reviewed and academic research papers, reputed organizations, research institutions, and medical associations to ensure accuracy and relevance. Read our editorial policy to learn more.
- Dairy Intake and Acne Vulgaris: A Systematic Review and Meta-Analysis of 78,529 Children, Adolescents, and Young Adults, Nutrients, US National Library of Medicine, National Institutes of Health.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6115795/ - A pilot study to determine the short-term effects of a low glycemic load diet on hormonal markers of acne: A nonrandomized, parallel, controlled feeding trial, United States Department of Agriculture.
https://pubag.nal.usda.gov/catalog/590455 - Acne and smoking, Dermato Endocrinology, US National Library of Medicine, National Institutes of Health.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2835905/ - What is the Role of Benzoyl Peroxide Cleansers in Acne Management?, The Journal of Clinical and Aesthetic Dermatology, US National Library of Medicine, National Institutes of Health.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3016935/ - Clinical studies of 20% azelaic acid cream in the treatment of acne vulgaris. Comparison with vehicle and topical tretinoin., Acta Dermato- venereologica, US National Library of Medicine, National Institutes of Health.
https://pubmed.ncbi.nlm.nih.gov/2528257/ - Treatment of acne vulgaris with salicylic acid pads., Clinical Therapeutics, US National Library of Medicine, National Institutes of Health.
https://pubmed.ncbi.nlm.nih.gov/1535287/ - An update on the management of acne vulgaris, Clinical, Cosmetic and Investigational Dermatology, US National Library of Medicine, National Institutes of Health.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3047935/ - Tretinoin: A Review of Its Anti-inflammatory Properties in the Treatment of Acne, The Journal of Clinical and Aesthetic Dermatology, US National Library of Medicine, National Institutes of Health.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3225141/ - Dual Effects of Alpha-Hydroxy Acids on the Skin, Molecules.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6017965/ - A Review of hormone-based therapies to treat adult acne vulgaris in women, International Journal of Women’s Dermatology, US National Library of Medicine, National Institutes of Health.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5419026/ - The efficacy of 5% topical tea tree oil gel in mild to moderate acne vulgaris: a randomized, double-blind placebo-controlled study., Indian Journal of Dermatology, Venereology, and Leprology, US National Library of Medicine, National Institutes of Health.
https://pubmed.ncbi.nlm.nih.gov/17314442/ - Witch-Hazel, ScienceDirect.
https://www.sciencedirect.com/topics/medicine-and-dentistry/witch-hazel - Formulation and Evaluation of Activated Charcoal Peel Off Mask, Research Gate, https://www.researchgate.net/publication/333130903_FORMULATION_AND_EVALUATION_OF_ACTIVATED_CHARCOAL_PEEL_OFF_MASK
- Bentonite Clay as a Natural Remedy: A Brief Review, Iranian Journal of Public Health, US National Library of Medicine, National Institutes of Health.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5632318/ - Origanum vulgare L. Essential Oil as a Potential Anti-Acne Topical Nanoemulsion—In Vitro and In Vivo Study
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6225355/ - Dietary water affects human skin hydration and biomechanics
https://pmc.ncbi.nlm.nih.gov/articles/PMC4529263/ - The Potential of Exercise on Lifestyle and Skin Function: Narrative Review
https://pmc.ncbi.nlm.nih.gov/articles/PMC10979338/ - The association between stress and acne among female medical students in Jeddah Saudi Arabia
https://pmc.ncbi.nlm.nih.gov/articles/PMC5722010/
Read full bio of Dr. Sruthi Alla
Read full bio of Ramona Sinha
Read full bio of Eshna Das
Read full bio of Krati Darak


























Community Experiences
Join the conversation and become a part of our empowering community! Share your stories, experiences, and insights to connect with other beauty, lifestyle, and health enthusiasts.