Perioral Dermatitis: 2 Home Remedies And Prevention Tips
Get rid of the rash and restore your skin back to life with some simple remedies.

Image: Shutterstock
Perioral dermatitis is often mistaken as acne around the mouth. However, it is a different condition, and you can easily get rid of perioral dermatitis at home. Sometimes it may extend to the nose or the eyes. In that case, it is called periorificial dermatitis.
While the exact cause of the rashes is not known, several factors may influence the occurrence of perioral dermatitis. Keep reading to understand the reason behind this condition, symptoms, home remedies, and treatment options.
In This Article
What Causes Perioral Dermatitis?

Many factors are thought to be responsible for the onset of perioral dermatitis. In most cases, it may be an after-effect of the products you use. Listed below are the most typical causes (1),(2),(3):
- Topical use of steroid creams and ointments
- Use of steroid sprays in the nose and mouth
- Overuse of heavy makeup, face creams, and moisturizers
- Use of fluoridated toothpaste
- Chewing gum
- Dental fillings
- Yeasts and bacteria that live on the skin and in hair follicles
- Hormonal changes
- Problems with the immune system
- Environmental factors, including exposure to UV rays
- Stress
- Poor hygiene
- Allergic reactions to medications
 Trivia
TriviaContinue reading to know the common signs and symptoms of perioral dermatitis.
Key Takeaways
- Perioral dermatitis is suspected to be caused by steroid use, adverse reactions to medications, stress, and more.
- People of various ages, races, and ethnicities can develop perioral dermatitis.
- However, it is most common in women between 20 and 45.
- Most home treatments, such as aloe vera and honey, can help supplement perioral dermatitis treatment.
- If you acquire an infection, see a doctor to get the appropriate treatment.
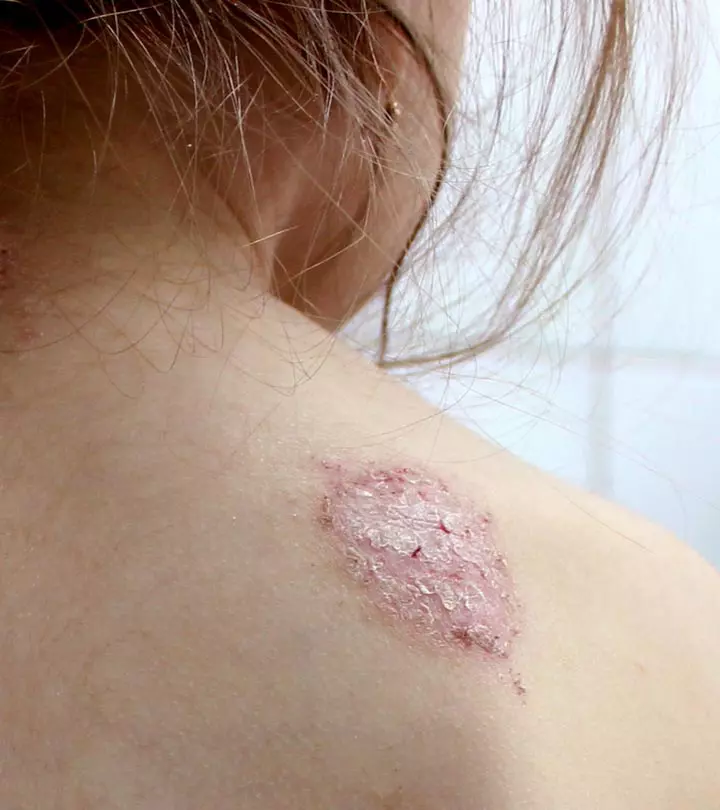
Symptoms Of Perioral Dermatitis
The skin condition is characterized by (1):
- Redness, scaly rash, and dry skin around the mouth; the rash may extend to the eyelids, nose, forehead, and genitals
- A burning sensation
- A tightening sensation on the skin around the mouth
- Watery discharge from the rashes
- Dryness and flakiness
- Tiny inflamed bumps or papules
- Vesicles or pustules (fluid-filled blisters)
- Itchiness
Let us find out who is more prone to perioral dermatitis in the following section.
Who Are Most Likely To Be Affected?
Perioral dermatitis can affect people of all ages, races, and ethnicities
. It can also affect children. However, it is most commonly observed in women aged between 20 and 45 (1).
Which parts of the face does perioral dermatitis affect? Keep scrolling to find out.
What Are The Most Affected Areas?
- Under the eyes
- Forehead
- Chin
- Around the mouth
Now that you know the spots that get hit the hardest, let’s talk about whether it can spread to others.
Is Perioral Dermatitis Contagious?
No, perioral dermatitis is not contagious. It is a non-infectious skin condition characterized by red, bumpy rashes around the mouth, nose, or eyes. Its exact cause is unclear, but it is not spread through contact with an affected individual.
So, can perioral dermatitis sort itself out?
Will Perioral Dermatitis Heal On Its Own?
Perioral dermatitis rarely heals on its own. While some mild cases may improve spontaneously, the condition often persists or worsens without treatment. Effective management usually requires medical intervention, such as topical or oral antibiotics. It’s essential to consult a dermatologist for an accurate diagnosis and personalized treatment plan, as neglecting it may lead to chronic or recurrent symptoms.
Read below how perioral dermatitis can be identified.
How Can Perioral Dermatitis Be Diagnosed?
- No tests are usually required to diagnose perioral dermatitis.
- Dermatologists can diagnose it by simply examining your face.
- They may enquire about the use of steroid creams and ointments apart from other pertinent histories. Or can suggest perioral dermatitis medication like oral antibiotics or topical creams.
- Swabs may be taken to run a skin culture to rule out an infection.
- In rare cases, your doctor may send a sample of the afflicted skin area to a dermatologist for a skin biopsy.
- The doctor may also conduct blood tests to rule out nutritional deficits.
The ingredients in your kitchen have a solution for most of your skin problems. Here, we bring to you a list of home remedies that may help complement the treatment for perioral dermatitis and help eliminate this condition.
Home Remedies For Perioral Dermatitis
Most topical skin care products contain the ingredients listed below. While these ingredients have not been evaluated for treating perioral dermatitis, they are thought to be beneficial for most types of dermatitis. These may help reduce the irritation, ease the symptoms, and heal the skin.
1. Aloe Vera

Aloe vera has anti-inflammatory, antimicrobial, and wound-healing properties. It may help soothe the skin and prevent further irritation if used daily (4).
How To Use?
- Apply pure aloe vera gel to the affected area.
- Allow it to absorb into your skin.
- Repeat every day.
2. Honey

Honey has scientifically been recognized for its antimicrobial and wound-healing properties. It helps treat facial redness, papules, pustules, and telangiectasia (tiny blood vessels causing threadlike red lines on the skin) (5).
How To Use?
- Apply raw honey to the affected areas.
- Wash off after half an hour.
- Repeat twice a day.
Note:
Discontinue these remedies immediately if you experience allergic reactions like continuous burning or increased redness.
While these remedies may be effective, they are not enough to alleviate this skin condition. Making changes to your skincare routine and lifestyle is also essential. Consider the following:
- Discontinue using steroid creams or sprays immediately.
- Skip heavy face washes and cream. Go for a gentle facial cleanser while your rash heals.
- Wash your hands before touching your face.
- Do not scrub the skin as it may cause more irritation.
- Avoid caffeine and alcohol.
- Change your pillowcase every day.
- Avoid chemical-based skin care products.
- Avoid face oils.
- Keep your body hydrated and eat a balanced diet.
Dani Marie, a blogger, discussed her personal experience with perioral dermatitis (POD). She found relief after using all-natural remedies and products with minimal to no chemicals. She said, “And when I stopped using any products on my face with “bad” ingredients, my pod cleared up (i)!”
Are these home remedies not working for you? Worry not. There are other treatment options available to control the symptoms and diminish the appearance of these rashes. Scroll down to know them.
Treatment Options Available For Perioral Dermatitis
According to a study, first-line treatment options for perioral dermatitis include metronidazole cream or gel, clindamycin lotion or gel, erythromycin gel, topical sulfur preparations, and azelaic acid gel. Antibiotics play a key role in treating this condition, thanks to their anti-inflammatory properties. Topical calcineurin inhibitorsi A type of medication that is used in the treatment of autoimmune and inflammatory diseases like lupus and atopic dermatitis. like tacrolimus ointment or pimecrolimus cream can also be effective.
Topical sulfur or sulfacetamide preparations and topical adapalene have also been demonstrated to show improvement. Besides, photodynamic therapyi A two-stage procedure that uses light energy to kill cancerous and precancerous cells after light activation. using 5-aminolevulinic acid as a photosensitizeri A chemical drug used in photodynamic therapy that becomes active and kills the cancer cells when it is exposed to light. has been found to be helpful. Oral antibiotics like tetracycline, doxycycline, and minocycline can be used to treat severe perioral dermatitis (1).
 Did You Know?
Did You Know?Do you need to see a doctor if you are affected by perioral dermatitis? Let’s find this out in the next section.
When Should You See A Doctor?

You should see a dermatologist right away as perioral dermatitis could be a sign of a more serious skin disease. Your dermatologist will be able to determine the severity of your illness and recommend an appropriate treatment for you.
But, as we know, prevention is better than cure. You can avoid many skin diseases by adopting a few preventive steps, and perioral dermatitis is no exception. Keep reading to know more.
Is It Possible To Prevent Perioral Dermatitis?

Here are a few steps to prevent perioral dermatitis:
- Avoid using topical steroids near the mouth and nose.
- Do not change any dermatologist-approved medication to steroids or stronger steroids.
- Do not use skin care products with harsh fragrances or surfactants if you have sensitive skin.
- Wearing masks may increase the risk of perioral dermatitis (6). Use clean masks.
- Avoid or remove heavy makeup before bed.
- Use sunscreen.
Infographic: Easy Remedies and Tips To Manage Perioral Dermatitis
Perioral dermatitis causes red, bumpy rashes around the mouth, nose, and chin. This condition can be improved with the help of natural remedies and following certain prevention tips. Check out the below infographic for some remedies and tips to help you manage the symptoms of perioral dermatitis.
Some thing wrong with infographic shortcode. please verify shortcode syntaxPerioral dermatitis is an inflammatory rash that appears around the mouth. It can also happen around the nose, chin, and eyes. The skin problem is more prevalent in adult women (20 to 45 years old) than men. While the actual cause of the rashes is unknown, perioral dermatitis can be influenced by several factors. It is often linked to topical steroids and the excessive use of makeup and other cosmetics. Take the safety precautions and treatment strategies suggested in the article into consideration. If you have an infection, see a doctor quickly away so they can prescribe the appropriate therapy.
Frequently Asked Questions
What triggers perioral dermatitis?
Perioral dermatitis can be triggered by factors like overuse of topical steroids, certain skincare products, hormonal changes, or stress.
How long does perioral dermatitis typically last?
With proper care and treatment, perioral dermatitis can improve in a few weeks, but more severe cases may take several months to clear completely.
Can diet affect perioral dermatitis?
Yes, some people find that certain foods, especially those high in sugar or spicy foods, can worsen symptoms. A balanced diet may help reduce flare-ups, though this can vary for each person.
Should I moisturize perioral dermatitis?
Yes, you can moisturize perioral dermatitis but ensure the natural remedy or moisturizer you use is gentle and light. Heavy or thick moisturizers may worsen this condition.
Is vitamin C good for perioral dermatitis?
You should consult a dermatologist before using vitamin C. Vitamin C may be too strong for perioral dermatitis and worsen the condition.
Is coconut oil good for perioral dermatitis?
Coconut oil may help with perioral dermatitis as it is antibacterial and moisturizing. However, there is a chance that it may clog pores and aggravate the condition.
Should you exfoliate perioral dermatitis?
No, you should not exfoliate the affected area as it can worsen the skin inflammation.
Is tea tree oil good for perioral dermatitis?
While tea tree oil has antimicrobial properties, it is not recommended to treat perioral dermatitis as it also has astringent properties that can strip off moisture and natural oils from your skin, leaving it dry.
Does perioral dermatitis come and go?
If left untreated, this condition can last for months or even years. It is recommended to go to a doctor, diagnose the cause, and get the right treatment to manage this condition.
Does taking zinc help perioral dermatitis?
If the condition is caused due to a zinc deficiency, taking zinc supplements can help,
Does petroleum jelly help perioral dermatitis?
Applying a thin layer of petroleum jelly can help by moisturizing the skin. However, do not slather on a thick layer of petroleum jelly or heavy cream as it can worsen the condition.
Say goodbye to perioral dermatitis with the secret cure revealed in this video. Learn effective methods to completely eliminate this skin condition in just four days.
Personal Experience: Source
StyleCraze's articles are interwoven with authentic personal narratives that provide depth and resonance to our content. Below are the sources of the personal accounts referenced in this article.
i. Let’s Start With A Success Story: How to Cure Perioral Dermatitis! https://sunshinefreedomalittleflower.wordpress.com/2012/03/08/lets-start-with-a-success-story-how-to-cure-perioral-dermatitis/References
Articles on StyleCraze are backed by verified information from peer-reviewed and academic research papers, reputed organizations, research institutions, and medical associations to ensure accuracy and relevance. Read our editorial policy to learn more.
- Perioral Dermatitis
https://www.ncbi.nlm.nih.gov/books/NBK525968/ - Perioral dermatitis from high fluoride dentifrice: a case report and review of literature
https://pubmed.ncbi.nlm.nih.gov/23981221/ - Psychological interventions in the management of common skin conditions
https://www.ncbi.nlm.nih.gov/labs/pmc/articles/PMC3218765/ - Pharmacological Update Properties of Aloe Vera and its Major Active Constituents
https://www.ncbi.nlm.nih.gov/labs/pmc/articles/PMC7144722/ - Honey: A Therapeutic Agent for Disorders of the Skin
https://www.ncbi.nlm.nih.gov/labs/pmc/articles/PMC5661189/ - Flare-up of Rosacea due to Face Mask in Healthcare Workers During COVID-19
https://pubmed.ncbi.nlm.nih.gov/33312262/
Read full bio of Dr. Anna H. Chacon
Read full bio of Monomita Chakraborty
Read full bio of Anjali Sayee
Read full bio of Swathi E
























Community Experiences
Join the conversation and become a part of our empowering community! Share your stories, experiences, and insights to connect with other beauty, lifestyle, and health enthusiasts.