Hidradenitis Suppurativa: Symptoms, Causes & Treatment Guide
Learning what triggers those painful bumps on the skin can help you choose the right treatment.

Image: Shutterstock
The red and painful bumps on your skin may not always be pimples. Instead, these skin breakouts on your neck, armpits, or groin could be a chronic skin condition called hidradenitis suppurativa. You may not have heard about this skin disease before, but it is one of the most unpleasant skin issues that may affect your quality of life. Though the exact cause of hidradenitis suppurativa is unknown, it is estimated that genetic, hormonal, and environmental factors may be responsible for it.
Have you noticed any such pimple-like bumps on your body? Are you wondering how to identify them? You have come to the right place. This article explores more about this condition and its symptoms and treatments. Keep reading!
 Trivia
TriviaIn This Article
What Is Hidradenitis Suppurativa?
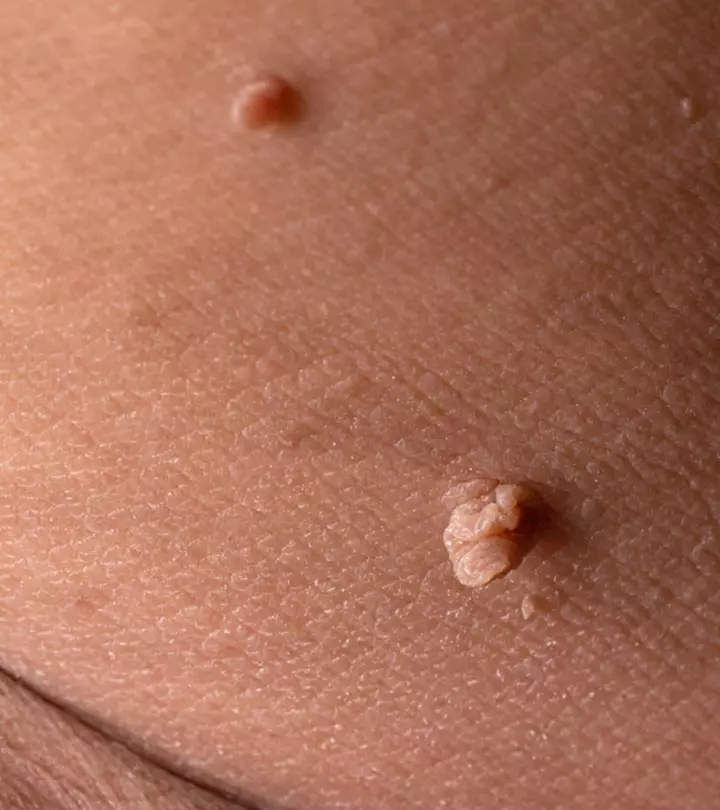
Hidradenitis suppurativa (HS), also known as acne inversa, is an inflammatory skin condition characterized by recurrent and painful pus-filled bumps that look like pimples and occur under the skin and fistulous tracts. It can occur in many forms, including deep acne-like nodules.
These lesions appear in areas rich in apocrine glands and where the skin rubs together, like your armpits, groin, under the breasts, ears, back of the neck, inner thighs, and buttocks.
This chronic condition is usually painful and affects up to 4% of the population. The acne-like nodules may rupture suddenly to form a painful and deep swollen lump filled with pus. Eventually, it may lead to scarring and sinus tract formation (1).
 Did You Know?
Did You Know?According to a study conducted in Canada, a hidradenitis suppurativa patient has some of the lowest quality of life measures than any other dermatologic disease (2). It can lead to psychological distress. Learn more about the symptoms of HS to get it treated to avoid further complications.
Key Takeaways
- Hidradenitis suppurativa is an inflammatory skin condition that occurs in areas where your skin rubs together, like the armpits, groin, and inner thighs.
- There are surgical and non-surgical treatments available to treat this skin condition.
- Recurrent breakouts and scarring may lead to other serious issues like skin cancer or physiological conditions like depression and anxiety.
What Are The Symptoms Of Hidradenitis Suppurativa?
Hidradenitis suppurativa begins with a painful skin breakout on the areas where the skin rubs together.
Its symptoms include:
- Painful, red lumps under the skin that get bigger and break open.
- Pockets of pus that itch and have an unpleasant odor.
- Small pitted skin with blackheads.
HS may heal very slowly and lead to scarring, abscesses, and tunnels under the skin. It can be mild, moderate, or severe. In mild HS, there may be only one or a few bumps in one area, but they often get worse. In moderate HS, the bumps keep recurring in more than one area on the skin. They may even become bigger and break open. Severe HS is characterized by widespread bumps, scarring, boils, and chronic pain. You may not even be able to move freely due to the pain. Stress, hormonal changes, heat, smoking tobacco, and obesity may worsen the condition too.
Fortunately, HS is not a contagious disease, but its cause is still not clear. Experts believe it could be due to several factors. Learn more about them in the next section.
What Causes Hidradenitis Suppurativa?

- Although the exact cause of HS is unknown, it is believed to be caused by blockages in hair follicles (not to be confused by the condition of folliculitis caused by inflamed hair follicles). The lesions can also develop due to excessive development of keratin in the hair follicles (3). The blocked hair follicles trap bacteria, lead to chronic inflammation, and rupture.
- Genetic, environmental, and hormonal factors are also suspected to be the reason behind HS. Approximately 33% of the cases are familial (4).
- Since HS occurs around puberty, there are also chances of hormones being one of the reasons for the development of HS (1).
Other possible associations of HS may be:
- Obesity
- Ulcers
- Smoking tobacco products
- Acne
- Abnormal sweat gland development
- Overactive immune system
- Any other inflammatory disease of the immune system
Anyone with these conditions is at an increased risk for HS. There are other factors that make certain groups vulnerable to HS. Learn more about them in the next section.
Who Is At Risk For Hidradenitis Suppurativa?

Your chances of developing HS may increase if you:
- Are in your 20s or 30s.
- Have severe acne, diabetes, arthritisi An inflammation, swelling, or stiffness of one or more joints, causing pain that worsens with age. , or other inflammatory diseases.
- Have a family history of HS.
- Are overweight or obese.
- Are a female.
- Are a current or past smoker.
If you have hidradenitis suppurativa, it is best to get yourself screened for other conditions, like depression, diabetes, or skin cancer, as well.
Getting it diagnosed at the right time will help you treat it effectively. Keep reading to find out how HS is diagnosed.
How Do Dermatologists Diagnose Hidradenitis Suppurativa?

Your doctor may do a physical examination of the bumps and ask about your medical history and symptoms. They may ask you questions about your family’s medical history as well. If your doctor has ruled out the possibility of any other infection, they will take a sample of skin or pus for testing.
Based on your symptoms and test results, the doctor will determine the stage and severity of your HS and plan the treatment accordingly. Read on to find out the treatment options for hidradenitis suppurativa.
What Are The Treatments For Hidradenitis Suppurativa?

There is no cure for this skin condition. However, treatment can help reduce the pain and severity of the breakouts, promote healing, and prevent further complications.
The treatment plan may include:
- Antibiotics: This is to reduce inflammation and bacterial infection and prevent new breakouts.
- Biologics: When topical medications and oral antibiotics fail or the disease has progressed, biological medications may be prescribed (4). It helps to suppress your immune system to prevent further breakouts and flare-ups.
- Biologics: When topical medications and oral antibiotics fail or when the disease has progressed, biological medications may be prescribed (4). It helps to suppress your immune system to prevent further breakouts and flare-ups.
- OTC Pain Relievers: You can take these to relieve the pain and discomfort caused by the breakouts.
- Retinoidsi A class of chemical compounds derived from vitamin A that help reduce skin discoloration and fine lines. : Topical or oral retinoidsi A class of chemical compounds derived from vitamin A that help reduce skin discoloration and fine lines. help treat acne and soothe the skin.
- Hormone Therapy: Studies have found hormone therapy to be an effective method for treating HS. Anti-androgen therapy appears to have an especially beneficial effect on HS treatment (5).
If your condition is severe and its symptoms keep recurring, your doctor may recommend surgical options to remove the lesions that have grown deep in your skin. Excision and unroofing (cutting away the skin that covers the tunnel) procedures are proven to be effective treatments with fewer complications and low recurrence rates (6). Other procedures include radiation and laser therapy.
To manage this condition in a better way, you may also try making some lifestyle changes, including:
- Quitting smoking.
- Maintaining a moderate weight by exercising regularly.
- Managing stress through mindfulness activities like yoga, meditation, journaling, etc.
- Avoiding sugary foods, dairy products, and brewer’s yeast.
- Wearing loose-fitting clothing.
- Laser-assisted hair removal.
- Regular application of body lotions.
Amy, a lifestyle blogger, recounted how she was diagnosed with and ended up treating HS. For her, the condition was caused by inflammation that she could control by making minor changes to her diet. But she mentions that this may not work for everyone. She writes, “The most frustrating part of Hidradenitis Suppurativa is finding out that what works for one sufferer does not necessarily work for another. For me, changing my diet has made all the difference in the world (i).”
 Quick Tip
Quick TipIf you do not take care of your symptoms and treat the condition, you may have to deal with the complications associated with HS. Learn more about them below.
What Are The Complications Associated With Hidradenitis Suppurativa?
The complications of HS include:

- Infection: The affected area may become infected if left untreated.
- Skin changes and scars: The bumps may heal but leave behind pitted scars, and your skin may become darker in color.
- Restricted movement: Painful sores and wounds may restrict your movement.
- Skin Cancer: Some people with advanced HS may develop skin cancer due to recurrent breakouts and scarring.
- Swelling In the arms, legs, or genitals: Bumps and scars that appear near lymph nodes may cause swelling.
- Psychological issues like anxiety and depression: The skin breakouts may lead to social isolation and loneliness.
The Bottom Line
Hidradenitis suppurativa is an inflammatory skin condition that affects the overall quality of a person’s life. If you notice symptoms related to HS, you should consult a doctor immediately. Though there is no cure for this condition, you can reduce its symptoms by getting timely treatment. Otherwise, it may lead to more complications, including skin cancer and psychological issues. The treatment includes antibiotics, biological medications, steroids, retinoidsi A class of chemical compounds derived from vitamin A that help reduce skin discoloration and fine lines. , and hormonal therapy. You may have to go for surgical options if the bumps keep recurring. Making the lifestyle changes mentioned above may also help improve your condition.
Frequently Asked Questions
Does hidradenitis suppurativa go away?
Even though there is no cure for hidradenitis suppurativa, early detection and treatment can help stop the condition from worsening and creating new scars.
Is hidradenitis suppurativa a STD?
No, hidradenitis suppurativa is not an STD. It can appear on the inner thighs near the genitals, leading some individuals to believe that HS is an STD or another contagious disease. However, people with HIV are prone to developing hidradenitis suppurativa (7). Usually, rashes are early symptoms of HIV. However, unlike HIV rashes that typically appear across the body, hidradenitis suppurativa presents as painful, inflamed nodules and abscesses in specific areas, such as the armpits and groin.
Does hidradenitis suppurativa shorten your life?
According to one study, hidradenitis suppurativa is frequently related to both spondyloarthritisi A group of diseases characterized by inflammation, pain, and stiffness in the spine and joints of the arms and legs. and metabolic changes, which raise the risk of cardiovascular disease and shorten life expectancy (8).
Can you give blood if you have hidradenitis suppurativa?
Yes, you can donate blood even if you have hidradenitis suppurativa. But some of the drugs and medications that you take for it may prevent you from doing so.
Can HS cause infertility in females?
A study found that hidradenitis suppurativa is linked to infertility in both males and females throughout all reproductive age groups, particularly in those between the ages of 36 and 45 and in female patients (9).
Illustration: Hidradenitis Suppurativa: Causes, Symptoms, And Treatment

Image: Dall·E/StyleCraze Design Team
Learn more about hidradenitis suppurativa. Get the facts on this painful skin condition and how to manage it effectively by watching this informative video.
Personal Experience: Source
StyleCraze's articles are interwoven with authentic personal narratives that provide depth and resonance to our content. Below are the sources of the personal accounts referenced in this article.
i. My HS Storyhttps://hidradenitishealing.blogspot.com/p/my-hidradenitis-suppurativa-story_9.html
References
Articles on StyleCraze are backed by verified information from peer-reviewed and academic research papers, reputed organizations, research institutions, and medical associations to ensure accuracy and relevance. Read our editorial policy to learn more.
- Hidradenitis suppurativa: a comprehensive review
https://pubmed.ncbi.nlm.nih.gov/19293006/ - Quality-of-life impairment in patients with hidradenitis suppurativa: a Canadian study
https://pubmed.ncbi.nlm.nih.gov/25432664/ - Hidradenitis suppurativa: Epidemiology clinical presentation and pathogenesis
https://pubmed.ncbi.nlm.nih.gov/31604104/ - Hidradenitis suppurativa: an update on connecting the tracts
https://www.ncbi.nlm.nih.gov/labs/pmc/articles/PMC5538037/ - Finasteride in Hidradenitis Suppurativa
https://www.ncbi.nlm.nih.gov/labs/pmc/articles/PMC4928456/ - Surgical Management of Hidradenitis Suppurativa: Outcomes of 590 Consecutive Patients
https://pubmed.ncbi.nlm.nih.gov/27340739/ - Hidradenitis Suppurativa in Patients with HIV: A Scoping Review
https://www.researchgate.net/publication/365012232_Hidradenitis_Suppurativa_in_Patients_with_HIV_A_Scoping_Review - Study Details Effects of Hidradenitis Suppurativa on QOL
https://www.ajmc.com/view/study-details-effects-of-hidradenitis-suppurativa-on-qol - The association between hidradenitis suppurativa and male and female infertility: A population-based study
https://pubmed.ncbi.nlm.nih.gov/33399222/
Read full bio of Dr. CP Thajudheen
Read full bio of Swathi E
Read full bio of Anjali Sayee
Read full bio of Monomita Chakraborty

























Community Experiences
Join the conversation and become a part of our empowering community! Share your stories, experiences, and insights to connect with other beauty, lifestyle, and health enthusiasts.