Red Circular Rash On Skin: 6 Conditions It Could Be
Be aware of the signs and possibilities to get the right line of treatment on time.

Image: Midjourney/ StyleCraze Design Team
Rashes with a circular border or a ring-like appearance are usually characteristic of and diagnostic of ringworm, a fungal skin infection (1). However, not every red circle on the skin may be a ringworm infection. Most of the time, people may confuse any red and circular rash with ringworm. That is why you should be aware of the symptoms and causes. This article will provide more information on the other skin conditions that could give you a similar red circle on skin. Read on.
In This Article
What Does The Red Circle On The Skin Mean?

Dr. Fayne Frey, MD, a dermatologist, says, “A red circle on the skin can be one of many things. Inflammatory conditions like atopic dermatitis or contact dermatitis may begin as a red circle. Certain infections like impetigo or fungal infection may begin as a red circle. Birthmarks, collagen vascular disease, bruising from trauma, and many other conditions can look like a red circle on the skin.”
A rash that is localized, with distinctive borders, is usually caused by certain external factors, while the rashes that seem red and inflamed that appear throughout the body are most often caused by internal conditions (2). Rashes like contact dermatitis and ringworm occur in response to external irritants (in skincare products, soaps, or detergents), allergens (in plants, food, and air), or organisms (fungus on our skin or (3), (4). On the other hand, rashes like atopic dermatitis or eczema that stem from internal abnormalities are usually due to genetics or when our immune system is overactivated by certain triggers (5).
When you get a red circular rash on your skin, you must first make sure whether it’s Ringworm or not. For that, you need to be aware of the characteristic features, types, and symptoms of Ringworm.
Key Takeaways
- You can get rashes due to external irritants and internal abnormalities.
- A ringworm infection is a common fungal skin infection that causes a ring-like circular rash that is red and itchy.
- Pityriasis rosea, contact dermatitis, nummular eczema, granuloma annulare, psoriasis, and lime disease also mimic ringworm infection.
What Is Ringworm? Types And Symptoms
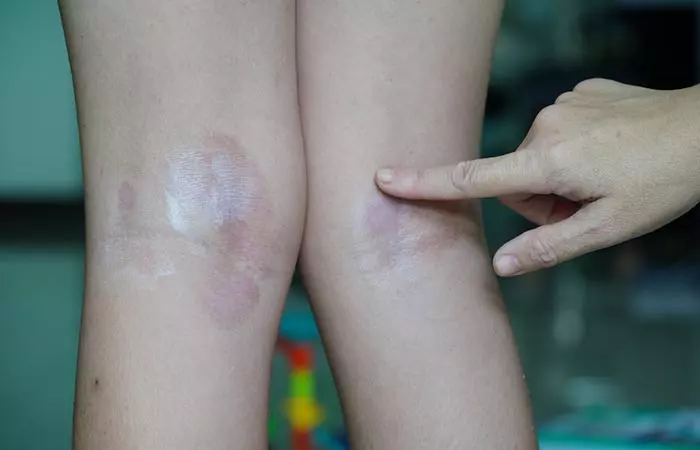
Ringworm, otherwise known as “tinea corporis” or “dermatophytosis”, is a common fungal skin infection. It is caused by a class of fungi called dermatophytes that feed on the dead cells of the skin, hair, and nails and tend to thrive in the warm, moist folds of the skin (6). Ringworm infection causes a characteristic itchy red circular rash. The circular itchy rash can have a red-colored center or a normal one of your skin color. Ringworm is further classified as per its location on the body (4).
- Tinea capitis
Ringworm of the scalp is known as Tinea capitis. It is usually seen in children in their growing years or around adolescence. It usually appears as scaly patches of balding spots on the scalp with a loss of hair. This ringworm might commonly spread from one child to another in their school (7).
- Tinea pedis
Commonly known as ‘Athlete’s foot’, Tinea pedis is the ringworm infection of the foot that causes scaling and inflammation in between the toes, especially the last two. It usually causes redness, itching, and burning sensation on the sole of the feet as well (8).
- Tinea manum
This affects the skin of the hand, especially in between the fingers. It usually leads to thickening of the skin in between the fingers (9). Tinea manuum is usually accompanied by Tinea pedis.
- Tinea unguium
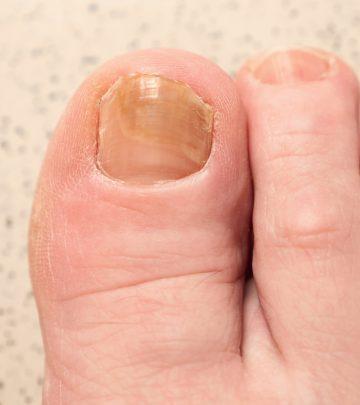
Ringworm of the nails is also a common occurrence. It causes the fingernails to look thick, white, opaque, and brittle, while the toenails appear yellow, thick, and brittle (10).
- Tinea barbae
This fungal infection of the beard on the face and neck results in swelling and marked crustings, often resulting in hair breakage (11). It was also commonly known as barber’s itch in earlier days when people used to visit the barber for haircuts and shave.
- Tinea faciei
Ringworm on the face, other than the beard, is known as Tinea faciei. It usually occurs as red scaly patches without a defined ring, and that might cause difficulty in its diagnosis (12).
- Tinea cruris
Commonly known as ‘Jock’s itch’, the tinea in the folds of the groin area usually appears as reddish-brown patches and might extend further down to the inner thighs (13). It is usually caused due to sweating or wearing tight clothes and can easily be confused with other yeast infections or psoriasis.
Since Ringworm is diagnosed through physical exams or fungal cultures, it is best to consult a doctor right at the beginning. Its treatment typically involves topical antifungal creams, like clotrimazole and ketoconazole. If topical treatments fail, let your doctor know immediately so they can set another course of treatment. In this case, they may also prescribe oral medications like terbinafine or itraconazole (4).
Ringworm is contagious and is often spread through contact. Household items, shared linen, or even pets and animals can transfer this fungal infection from one person to another.
If It’s Not Ringworm, Then What Else Could It Be?
 Quick Tip
Quick Tip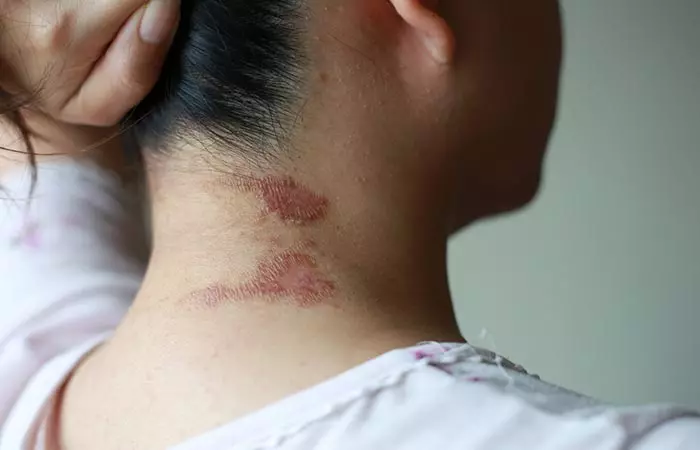
A ring-like circular rash similar to ringworm, in certain cases, might get diagnosed as some other skin condition. Since these would require a different line of treatment, it is vital to get the correct diagnosis done in consultation with your medical practitioner (2).
A few of the skin conditions that commonly mimic ringworm are as follows:
- Pityriasis rosea
Pityriasis rosea is a common and benign rash that appears red, scaly, and itchy. It typically starts as one single large spot known as the ‘herald patch’ on the back, chest, or abdomen, and is then commonly followed by more small patches or bumps in a pattern that resembles a pine tree (14, 15). It is, in the absence of this big red circle on skin, when the diagnosis might get difficult. It usually resembles ringworm and you might feel unwell for a day or two before it shows up. Human Herpes Virus (HHV-7 and HHV-6) have been implicated as the causative agent in most cases but the cause remains largely unclear (16).
Pityriasis rosea is diagnosed using dermatoscopy, allowing dermatologists to observe the infection’s characteristic features, such as scaling patterns and the shape and arrangement of lesions. It is a self-limiting skin condition that typically resolves on its own and requires the use of moisturizers, switching to gentle soap alternatives, and getting limited sun exposure. However, it is best to consult a doctor if the condition causes significant discomfort. In some cases, doctors may prescribe certain medications, like macrolides or acyclovir, that speed up the healing process and reduce itching (17).
 Trivia
Trivia- Contact Dermatitis
Contact dermatitis is a kind of eczema and/or allergy that is usually a reaction to when the skin comes in contact with certain irritants in soaps and cosmetics, detergents, or materials like metals or latex (18). It can also refer to the more common ‘diaper rash’ or the skin peeling and cracking due to excessive handwash. Since contact dermatitis causes patches of thickened scaly skin, it tends to get confused with ringworm easily.
Its diagnosis involves patch testing that helps identify specific allergens or irritants responsible for the reaction. During the procedure, small amounts of potential allergens are applied to patches and adhered to the skin. The area is then checked for signs of redness, swelling, or rash to confirm sensitivity. Its treatment includes avoiding triggers or allergens, using moisturizers, and applying topical corticosteroids like clobetasol propionate 0.05% cream. Immediately consult your doctor if the rash persists, worsens, or shows signs of infection (3).
- Nummular Eczema
Nummular eczema is another skin condition that is commonly mistaken as ringworm. ‘Nummular’ means ‘coin’ in Latin and this rash is known to appear as coin-shaped patches of dry and scaly skin with variable levels of irritation, itching, and burning sensation. Bug bites, medications, and contact with metals such as nickel are known to be common triggers. It is usually aggravated by soaps, cosmetics, and abrasive fabric like wool (19).
Nummular eczema is diagnosed through a dermoscopy, a skin imaging technique that uses a handheld device to examine the rashes (19). Its management focuses on protecting and repairing the skin using ceramide moisturizers, hydrating soaps, etc. It is also recommended to avoid irritants like tight clothing and scratchy fabrics. You should seek medical attention if the symptoms persist or become widespread. In this case, the doctor may prescribe topical treatments, such as corticosteroid creams, to reduce redness and itching. For stubborn cases, light therapy or systemic treatments like oral steroids may be recommended (20).
- Granuloma Annulare
Another common ringworm-like skin condition that appears as raised, flesh-colored rings is Granuloma annulare. These bumps may show up on any part of the body and are, most often, localized in one area. The patches may look red to start with but that disappears once the ring forms. The rings could be ¼ of an inch- 2 inches in diameter. There is usually no itching or scaling. While the exact cause has not been established yet, in certain cases, it is associated with diabetes, thyroid, and trauma (21).
A skin biopsy may be required to diagnose these red circles on the skin. Mild cases resolve on their own but are prone to reoccurrence. While there is limited scientific evidence supporting treatments, doctors use various options for cosmetic or healing purposes based on the cause. Steroid injections are the most common and effective treatment. Other methods, like light therapy and certain medications like hydroxychloroquine, have also shown some success (22).
According to a study, women are more likely to be affected by Granuloma Annulare than men. The estimated prevalence and incidence of the condition are reported to be 0.1% to 0.4%. While more than two-thirds of patients dealing with this condition are 30 or less than 30, it can affect a person at any age.
- Psoriasis
Psoriasis is an auto-immune condition in which the immune system attacks its skin cells, leading to hyperproduction and inflammation. New skin cells get overproduced before the old ones can be shed off resulting in thick, scaly inflamed skin patches. These might itch or get sore with bleeding when scratched. This chronic condition is usually triggered by stress, medications, infections, environmental factors, or injury (23). Since Psoriasis resembles a few other skin conditions, and a blood test can’t establish the same, a skin biopsy might be prescribed for a confirmed diagnosis (24).
Topical therapies are the first line of treatment for mild to moderate psoriasis. This may include emollients and moisturizers that help maintain skin hydration and topical agents like corticosteroids and retinoids. If these treatments do not work, your doctor may also prescribe medications like methotrexate and cyclosporine (24).
- Lyme Disease
Lyme disease is caused due to tick bites and is usually manifested early on as a round red rash (shaped like a bull’s eye) called erythema migrans. This is a classic symptom found in over 70% of the cases and treatment is usually started just based on the same (25). Typically, it occurs as one lesion but in some cases, people might also have multiple lesions. The rash usually appears after 7-14 days but can show up as early as 3 days or as later as 32 days. The rash tends to expand in size without proper treatment. Early diagnosis and treatment help prevent the chronic effects that are usually seen later on in the disease.
Lyme disease can be difficult to diagnose as many patients do not remember being bitten by a tick or noticing a rash, and its symptoms are often vague. The CDC recommends a two-step blood test for its diagnosis. The first test screens for antibodies to the bacteria causing Lyme disease. If the result is positive or unclear, a second test called the Western blot test is used. It is important to note that blood tests may be unreliable in the early stages of infection because it takes time for the body to produce antibodies (26).
 Did You Know?
Did You Know?When To See A Doctor For Red Circles On The Skin?

Rashes on the skin tend to resolve on their own in little time. But it is important to get a professional opinion when they take more time to resolve or you notice any unusual changes. Even though a red circular rash is characteristic of Ringworm, occasionally, it could be something more serious. It is always better to get a rash examined by a doctor, to be able to follow the correct line of treatment.
Treatment For Red Circles On Skin
When you get a red circular rash on your skin, it is important to establish whether it is Ringworm or any of the other skin conditions mentioned above. This can only be done through proper diagnosis by your Dermatologist. Based on the diagnosis, the line of treatment would then vary accordingly.
Ringworm or most Tinea infections are superficial fungal infections that can usually be treated with topical antifungal creams, lotions, or powders in about 2-4 weeks. Non-prescription OTC products like Clotrimazole, Miconazole, Terbinafine, Ketoconazole can be helpful in treating Ringworm by following the dosage instructions on the package. You would need to get in touch with your dermatologist if the infection seems to be getting worse (27). Oral antifungals might then be prescribed to resolve the infection better.
In rashes like contact dermatitis, eczema, and Lyme disease that are caused by external factors (chemical irritants, allergens, or micro-organisms), it is helpful if one can identify and remove the triggers from the surroundings. These are usually treated with alcohol-free moisturizers, warm baths, topical corticosteroidsi Anti-inflammatory drugs that aid in the suppression of an overactive immune system and treating skin infections and allergic reactions. , antihistaminesi Medications used to treat allergies, skin reactions, and insect bite irritation, and sometimes used in the treatment of conjunctivitis. , and antibiotics (3), (5), (26). Pityriasis Rosea is usually treated with topical steroids or antihistamines, to reduce the itchiness and discomfort in general (28).
Any rash that’s caused due to internal causes would require a more intensive treatment rather than just topical creams and lotions. For instance, Psoriasisi An autoimmune skin condition that typically affects the scalp, elbows, and knees and causes red, scaly, and patchy skin. can sometimes resolve on its own but most often, is managed with topical steroids, Immunosuppressants, and UV light therapy (29). In the case of Granuloma annulare, the rings often disappear on their own in a few months and may not require any treatment. But sometimes, these lesionsi When a specific area of the skin is injured or damaged, causing the tissue to deteriorate and become abnormal. might get widespread and require medical consultation for a more intensive line of treatment (22).
In all the above, the doctor can also help diagnose if the rash involves any other kind of infection or potential complications and might prescribe antibiotics or other lines of treatment as deemed suitable. In case of less severe conditions, you may try the natural remedies mentioned below to treat red circles or for temporary relief.
Home Remedies For Red Circles On The Skin
- Cold Compress: Apply a cold cloth or ice pack to the affected area to soothe it and minimize inflammation.
- Aloe Vera Gel: Apply fresh aloe vera gel to the affected area. Its soothing and anti-inflammatory properties can reduce redness and irritation (30).
Tracie Dang, a vlogger, shared about using fresh aloe vera to reduce her red rashes in her video. She said, “My skin has cleared up so much. Especially my arms. It has cleared up all over (i)”
- Cucumber Slices: Place cucumber slices on the affected area to reduce redness and puffiness (31).
- Tea Tree Oil: Apply diluted tea tree oil to the affected area. The oil has antiseptic properties that can combat infections and reduce redness (32).
- Apple Cider Vinegar: Applying diluted apple cider vinegar to the affected area can help. The vinegar may help ease inflammation (33).
Always perform a patch test before applying any remedy. Although home remedies may provide some relief, it is advisable to consult a healthcare professional if the red circles persist or worsen. This is because specific treatments may not be effective for all skin types or conditions.
Infographic: Skin Conditions That Might Cause Circular Rashes
If the red patches on your skin do not go away by themselves in a day or two, they might be hinting at an underlying condition. A ringworm is fairly simple to recognize, but there are also other conditions that manifest in the same way and their diagnoses, treatment, and effects may vary. Identifying the type of condition is the first step towards appropriate treatment. Find below an infographic with a summary of all skin conditions that appear as red circular patches.
Some thing wrong with infographic shortcode. please verify shortcode syntaxEvery red circle on the skin may not be a ringworm infection. The size, location, color, shape, and texture of the red rash will help you identify the type of rash and diagnose it. You can get a red rash due to internal and external reasons. Pityriasis rosea, contact dermatitis, eczema, psoriasis, Lyme disease, etc., are the other skin conditions where the symptoms mimic a ringworm infection. In some cases, you may experience other symptoms like breathing issues or headaches along with red rashes. It is always best to consult a doctor if you experience these issues. With a timely diagnosis, it will be easy to treat the condition.
Frequently Asked Questions
When should I be worried about a red spot?
A red spot on the face can have many causes. Dr. Frey says, “Like any skin condition, if it lasts longer than a week or if it is causing symptoms like pain, itching, burning, I always advise the person to see a dermatologist.”
Can ringworm be misdiagnosed?
According to Dr. Frey, “Yes, since tinea corporis, also known as ringworm, can present as a simple red circle, it can be misdiagnosed.”
What precautions should I take when treating a red circular rash at home?
When treating a red circular rash at home, it is important to keep the affected area clean and dry. Gently wash the area with mild soap and lukewarm water, then pat it dry. Using an over-the-counter antifungal cream can help fight infection or reduce inflammation, but make sure you carefully follow the instructions given on the product. To prevent more irritation or infection, avoid scratching the rash; instead, apply cool compresses to reduce redness and itching.
Can stress cause red circles on the skin?
Stress may cause rashes on the skin (called hives). It may also worsen existing conditions like eczema or psoriasis.
What does a bacterial circle rash look like?
The bacterial rash will have a red center surrounded by a clear ring of red bumps.
What can it be if the red circle on the skin is not itchy?
Sometimes the rash looks like ringworm but is not itchy. Then, it could be psoriasis or eczema. As discussed above, the symptoms are similar. Therefore, always consult a doctor and get it diagnosed before starting any treatment.
Personal Experience: Source
StyleCraze's articles are interwoven with authentic personal narratives that provide depth and resonance to our content. Below are the sources of the personal accounts referenced in this article.
i. Aloe Vera Gel for Skin Rasheshttps://www.youtube.com/watch?v=wgX4wSIL4M4
References
Articles on StyleCraze are backed by verified information from peer-reviewed and academic research papers, reputed organizations, research institutions, and medical associations to ensure accuracy and relevance. Read our editorial policy to learn more.
- Ringworm
https://www.cdc.gov/fungal/diseases/ringworm/index.html - The Generalized Rash: Part I. Differential Diagnosis
https://www.aafp.org/pubs/afp/issues/2010/0315/p726.html - Contact Dermatitis
https://www.ncbi.nlm.nih.gov/books/NBK459230/ - Tinea Corporis
https://www.ncbi.nlm.nih.gov/books/NBK544360/ - Eczema
https://www.ncbi.nlm.nih.gov/books/NBK538209/ - Ecology and epidemiology of dermatophyte infections
https://pubmed.ncbi.nlm.nih.gov/8077503/ - Tinea Capitis
https://www.ncbi.nlm.nih.gov/books/NBK536909/ - Tinea Pedis
https://www.ncbi.nlm.nih.gov/books/NBK470421/ - Tinea Manuum
https://www.ncbi.nlm.nih.gov/books/NBK559048/ - Tinea Unguium Onychomycosis Caused By Dermatophytes: A Ten-year (2005–2014) Retrospective Study In A Tertiary Hospital In Singapore
https://www.ncbi.nlm.nih.gov/labs/pmc/articles/PMC6199187/ - Tinea Barbae
https://www.ncbi.nlm.nih.gov/books/NBK563204/ - Mycological And Clinical Aspect Of Tinea Faciei: A Ten-year Study
https://www.researchgate.net/publication/284409596_Mycological_and_clinical_aspect_of_tinea_faciei_A_ten-year_study - Tinea Cruris
https://www.ncbi.nlm.nih.gov/books/NBK554602/ - Pityriasis Rosea: An Updated Review
https://pubmed.ncbi.nlm.nih.gov/32964824/ - Herald Patch
https://pubmed.ncbi.nlm.nih.gov/30020673/ - Human Herpesviruses 6, 7, And 8 From A Dermatologic Perspective
https://www.ncbi.nlm.nih.gov/labs/pmc/articles/PMC3538396/ - Pityriasis Rosea
https://www.ncbi.nlm.nih.gov/books/NBK448091/ - Allergic Contact Dermatitis
https://www.researchgate.net/publication/8354799_Allergic_Contact_Dermatitis - Nummular Eczema: An Updated Review
https://pubmed.ncbi.nlm.nih.gov/32778043/ - Nummular Dermatitis
https://www.ncbi.nlm.nih.gov/books/NBK565878/ - Granuloma Annulare
https://pubmed.ncbi.nlm.nih.gov/26487494/ - Granuloma Annulare
https://www.ncbi.nlm.nih.gov/books/NBK459377/ - Causes – Psoriasis
https://www.nhs.uk/conditions/psoriasis/causes/ - Psoriasis
https://www.ncbi.nlm.nih.gov/books/NBK448194/ - Lyme Disease In Humans
https://www.ncbi.nlm.nih.gov/labs/pmc/articles/PMC7946767/ - Lyme Disease
https://www.ncbi.nlm.nih.gov/books/NBK431066/ - Treatment of Ringworm and Fungal Nail Infections
https://www.cdc.gov/ringworm/treatment/index.html - Pityriasis Rosea: Diagnosis And Treatment
https://www.aafp.org/pubs/afp/issues/2018/0101/p38.html - Psoriasis: A Review Of Existing Therapies And Recent Advances In Treatment
https://www.researchgate.net/publication/328138246_Psoriasis_A_Review_of_Existing_Therapies_and_Recent_Advances_in_Treatment - The Effect of Aloe Vera Clinical Trials on Prevention and Healing of Skin Wound: A Systematic Review
https://pmc.ncbi.nlm.nih.gov/articles/PMC6330525/ - Phytochemical and therapeutic potential of cucumber
https://pubmed.ncbi.nlm.nih.gov/23098877/ - Efficacy and safety of Melaleuca alternifolia (tea tree) oil for human health—A systematic review of randomized controlled trials
https://www.frontiersin.org/journals/pharmacology/articles/10.3389/fphar.2026.1116077/full - Antimicrobial activity of apple cider vinegar against Escherichia coli, Staphylococcus aureus and Candida albicans; downregulating cytokine and microbial protein expression
https://pmc.ncbi.nlm.nih.gov/articles/PMC5788933/
Read full bio of Dr. CP Thajudheen
- Dr. Fayne Frey is a board-certified dermatologist with 13 years of experience. She is a graduate of Boston University and the Weill Cornell Medical College. She is also a fellow of the American Academy of Dermatology and the American Society for Dermatologic Surgery.
 Dr. Fayne Frey is a board-certified dermatologist with 13 years of experience. She is a graduate of Boston University and the Weill Cornell Medical College. She is also a fellow of the American Academy of Dermatology and the American Society for Dermatologic Surgery.
Dr. Fayne Frey is a board-certified dermatologist with 13 years of experience. She is a graduate of Boston University and the Weill Cornell Medical College. She is also a fellow of the American Academy of Dermatology and the American Society for Dermatologic Surgery.
Read full bio of Eshna Das
Read full bio of Anjali Sayee
Read full bio of Swathi E


























Community Experiences
Join the conversation and become a part of our empowering community! Share your stories, experiences, and insights to connect with other beauty, lifestyle, and health enthusiasts.