Ulcerative Colitis Rash: Causes, Symptoms, & How To Manage It
This long-term condition causes skin problems, but there are easy ways to manage them.
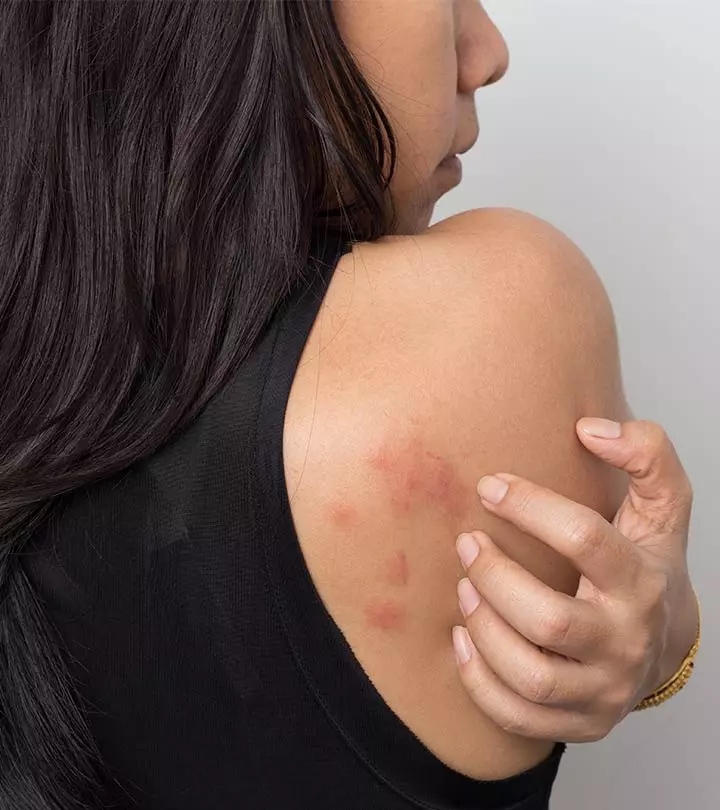
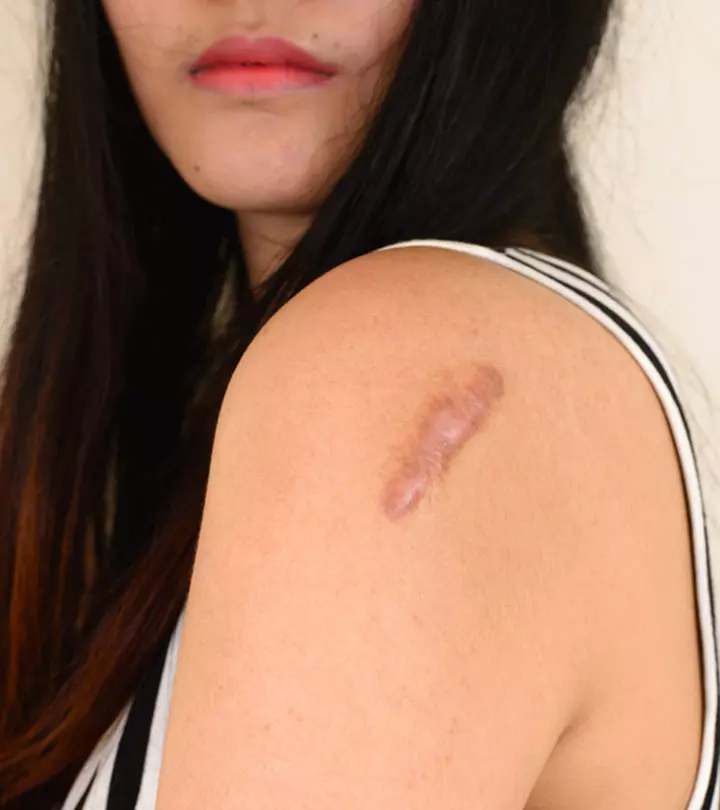
Image: Shutterstock
Anyone with inflammatory bowel disease (IBD) knows how unpleasant ulcerative colitis rash can be.
IBD is a condition in which the digestive tract is affected, and the exact cause of this ailment is unknown. Ulcerative colitis is a type of IBD that not only affects your digestive tract (the large intestine) but can also cause many skin issues (1). Such skin problems can make you more uncomfortable and even cause pain. Such skin problems can make you more uncomfortable and even cause pain. Thus recognizing the link between ulcerative colitis and skin issues can help individuals pursue proper treatment and make necessary life changes. In this article, we look at the effects of ulcerative colitis rash and explore ways to treat it. Keep reading!
In This Article
Colitis Vs. Ulcerative Colitis
Colitis generally refers to any inflammatory condition occurring in the lining of the large intestine or colon. The inflammation may be caused by radiation, surgery, medication aftereffects, etc. It can also be caused by a bacterial, viral, or parasitic infection. Less severe forms of colitis may be managed with diets, medication, and surgeries.
Ulcerative colitis is a specific, chronic, inflammatory bowel disease that occurs in the innermost lining of the colon and rectum. What causes it is unclear. But medical science identifies genetics and environmental and autoimmune factors as triggers. This condition requires long-term management that involves medication, an ulcerative colitis diet, and lifestyle modifications.
In either case, it is recommended to have the symptoms thoroughly evaluated by a medical professional for effective treatment. Let’s now dive deeper into the etiology of ulcerative colitis.
Key Takeaways
- Ulcerative colitis may also cause skin rashes.
- Other skin issues it may potentially cause include hives, acne, vitiligo, and psoriasis.
- In most cases, treating ulcerative colitis can help reduce the other associated symptoms.
- Keeping the affected area clean and following a balanced diet are important.
- Your doctor may also prescribe corticosteroids to reduce the inflammation.
Ulcerative Colitis And Skin Rashes: The Causes
Several kinds of rashes are associated with ulcerative colitis, an inflammatory condition that affects the large intestine. You may experience painful red rashes on the skin. These are triggered by the inflammation within your body and may appear as a medication side effect.
Ulcerative colitis is also associated with skin irritation and issues like psoriasis, vitiligo, pyoderma gangrenosum, dermatosis, erythema nodosum (bruise-like painful rashes), and acquired epidermolysis bullosa (skin blisters). These issues often result from inflammation and problems associated with the immune system mechanism related to IBD. Immunodeficiency is a common concern for people with inflammatory bowel diseases like ulcerative colitis (1), (2).
Ulcerative colitis is also associated with Sweets syndrome (1). This rare inflammatory condition causes rashes on body parts like the arms, legs, trunk, face, and neck. Patients on immunosuppressive therapy may experience it when the therapy is intensified.
Knowing just the causes is not enough to treat the condition effectively. You also need to know the symptoms, as discussed below.
Signs And Symptoms Of Ulcerative Colitis

The intensity and seriousness of ulcerative colitis symptoms vary among the people affected by the condition. While some people may experience periods of mild symptoms, some might experience no symptoms at all.
However, the return of symptoms is quite common, and you may experience them during a flare-up. The common symptoms include (3):
- Mild to severe abdominal pain
- Diarrhea
- Increase in abdominal sounds
- Fever and rectal pain
- Blood in stools
- Sudden weight loss
- Itchy bumps and hives
- Changes in skin pigmentation
- Red lesions
Apart from these, ulcerative colitis may also cause:
- Joint swelling and pain
- Nausea
- Reduced appetite
- Ulcers and mouth sores
- Eye inflammation
One of the other important aspects of handling skin issues associated with ulcerative colitis is to know the various skin conditions caused by it. These are discussed in the next section.
Skin Conditions Associated With Ulcerative Colitis
1. Erythema Nodosum
About 3% to 10% of the people with this ulcerative colitis may develop erythema nodosum in any body part. This is a condition in which you develop red and tender nodules on the skin.
The lesions may have a bruise-like appearance, and they can appear anywhere there is subcutaneous fat (the type of fat that sits right under the skin). The most common areas where you can develop erythema nodosum are the ankles, arms, shin area, knees, and trunk (1).
To ease the pain related to the condition, keep your legs elevated and apply a cool compress. In severe cases, pain relievers such as ibuprofen or naproxen may help.
 Quick Tip
Quick Tip2. Pyoderma Gangrenosum
This is the next most common skin condition that affects people with ulcerative colitis (1). A study conducted in 2011 involving 950 patients demonstrated that about 2% of them developed pyoderma gangrenosum (4).
This condition causes noninfectious nodules (blisters) on your skin. These eventually spread and develop into deep ulcers with wound edges. They can appear anywhere on your skin but mostly occur on the extensor surface of the legs (the side opposite to the joints), such as the shins and ankles. They may also appear on the extensor surfaces of your arms.
This condition is thought to be caused by immune system dysfunction. Usually, high doses of corticosteroids and other drugs are used to suppress your immune system to heal these wounds (1).
3. Hives

Hives are raised bump-like rashes on the skin that are itchy. These usually occur as a side effect of certain medicines you might be taking for ulcerative colitis. These can appear on any body part. If you feel that any medication is causing these reactions, consult your doctor immediately and ask for an alternative.
4. Fissures
IBD can also cause small tears or fissures in the skin around your anus. This can lead to blood in your stool and pain during bowel movement. While most of these tears heal on their own, warm baths and ointments can help ease the pain or itchiness.
If the fissure persists, doctors may prescribe various medicines to help relax the muscles in the affected area and promote fast healing (5).
5. Psoriasis
Psoriasis is a condition in which skin cells’ production speeds up, causing an excess buildup of cells on the skin surface. As a result, your skin looks scaly, with red patches all over the affected area. This is an autoimmune disorder and can also be triggered by ulcerative colitis. A study found a prevalence of psoriasis in 5.7% of 88 patients with ulcerative colitis (6), (7).
6. Acne
Ulcerative colitis may also cause cystic acne. This is the most severe form of acne and can be painful. A study found that using isotretinoin for cystic acne might aggravate ulcerative colitis symptoms (8).
In other words, if you have ulcerative colitis or are at risk of developing this condition, and if you have cystic acne, taking this drug may worsen the symptoms of ulcerative colitis.
7. Vitiligo

This is a condition in which your skin loses its color. The cells (melanocytes) that produce melanin and are responsible for your skin color start dying or stop functioning. As a result, you get white patches on the affected area.
According to a study led by Richard Spritz, M.D., Director of the Human Medical Genetics Program, University of Colorado, the onset of vitiligo is very highly associated with other autoimmune diseases (9), (1).
8. Pyodermatitis-Pyostomatitis Vegetans
These are two different skin conditions pyodermatitis vegetans and pyostomatitis vegetans.
Pyodermatitis vegetans is a very rare skin disorder in which you develop red pustules on the skin, which can easily rupture and form plaques or patches. It usually occurs in your skin folds, such as the groin or the armpits.
Similarly, in pyostomatitis vegetans, you get pustules in the mouth. The symptoms of both these conditions appear after you have had ulcerative colitis for a few years (1).
9. Sweet’s Syndrome
This is a very rare skin condition. You get painful skin lesions along with fever. The lesions look like red patches or clusters of red, painful bumps. These mostly appear on your head, neck, trunk, and arms. The exact cause of this skin disease is unknown. There are very rare cases (approximately 40) where researchers found a link between ulcerative colitis and Sweets syndrome (10), (11).
10. Bowel-Associated Dermatosis-Arthritis-Syndrome (BADAS)
This is a condition in which you develop lesions or pustules in areas such as the arms, upper chest, and legs. If you have Inflammatory Bowel Disease (either Crohn’s disease or ulcerative colitis), you are more likely to develop BADAS (12), (13).
11. Leukocytoclastic Vasculitis
In this condition, the small blood vessels under your skin become inflamed. As a result, they burst and create a pool of blood under your skin. This creates reddish-purple spots on your skin, also known as purpura. These are usually found on your legs and ankles. Typically, these spots go away once your ulcerative colitis symptoms are gone.
These skin rashes are usually caused due to inflammation within your body. However, some skin issues are caused as a side effect of the medicines you are taking for ulcerative colitis.
But is there any way to manage these issues?
Managing And Treating Skin Problems Caused By Ulcerative Colitis:
All of the above skin issues are related to ulcerative colitis, so the best way to manage them is to treat the underlying condition. Most of the time, you get skin rashes only during ulcerative colitis flare-ups. It is best to keep the condition in control to avoid getting these associated skin issues.
Ulcerative colitis-related issues are diagnosed with a combination of X-rays, blood tests, and stool tests. Alternatively, various medical imaging tests, such as MRIs, CT scans, and MRIs, are conducted for diagnosis.
During a flare-up, you can take these measures to avoid skin issues:
- Take the prescribed corticosteroid to reduce the inflammation.
- Keep your skin or the affected area clean to reduce the chances of infection.
- Follow a well-balanced diet. Vitamins and nutrients are essential for your skin health.
- Keep open wounds, lesions, or patches (due to the skin disorder) covered with bandages.
- Use a doctor-prescribed topical ointment or pain medication to manage discomfort.
Usually, doctors prescribe corticosteroids to manage skin inflammation. However, there could be more to skin inflammation; hence, knowing everything about it is crucial. It helps you better pinpoint the exact reason and take the proper medication to treat it.
 Quick Tip
Quick TipDiet plays a big role in the management of IBDs such as ulcerative colitis. Parker Lyons, a blogger, emphasizes the same in his blog while discussing his journey of fighting multiple health disorders, ulcerative colitis being one of them. He writes,“Food provided me with the energy and physique that allowed me to remain happily active and contributed greatly to my overall sense of fulfillment even with complications related to ulcerative colitis (i).”
Skin rashes and other complications associated with ulcerative colitis improve once the underlying causes are treated. Doctors may prescribe topical or oral steroids, antibiotics, and immunosuppressant medicines, depending on your condition.
To be prepared to deal with ulcerative colitis skin rashes, it is important to know who is prone to develop the condition. Read on to know more.
Who Gets Ulcerative Colitis?
Anyone can develop ulcerative colitis. However, you are at a greater risk of developing the condition if:
- You have a family history of IBD.
- You consume a high-fat diet.
- You take nonsteroidal anti-inflammatory drugs (NSAIDS).
Infographic: Foods To Eat And Avoid With Ulcerative Colitis
It is important to pay attention to your diet if you have ulcerative colitis (UC). Certain foods can trigger UC flare-ups. So how can you avoid those foods while still getting enough nutrients? A diet plan can be beneficial in this situation.
There is no specific diet that can treat UC for everyone. Since the condition can change over time, your plan must be adaptable as well. The important thing is to figure out what works best for you. Before beginning any diet, it is good to talk to your doctor about your triggers. Listed in the infographic below are some foods to eat and avoid if you have ulcerative colitis. Check it out!
Some thing wrong with infographic shortcode. please verify shortcode syntax
Ulcerative colitis is an inflammatory bowel disease that affects the large intestine, resulting in chronic inflammation, and causes red, painful rashes on the skin called ulcerative colitis rashes. Ulcerative colitis rash may be accompanied by gastrointestinal symptoms such as abdominal pain, diarrhea, and other symptoms like nausea, eye inflammation, and sudden weight loss. Ulcerative colitis is associated with a range of skin conditions such as eczema, psoriasis, hives, and acne. You can resort to prescribed corticosteroids to rescue the inflammation. Other than this, a balanced diet and keeping clean skin can help manage the condition better. Consult a doctor for proper diagnosis and treatment.
Frequently Asked Questions
How do you know if your ulcerative colitis is flaring up?
Abdominal pain, cramping, bleeding, fatigue, diarrhea, rectal bleeding and pain, and urgent bowel movements are signs of ulcerative colitis flare-up.
Can ulcerative colitis be transmitted?
No, ulcerative colitis cannot be transmitted.
Is ulcerative colitis caused by a virus?
The cause of ulcerative colitis is still unknown. It can be caused by a bacteria or virus.
How serious is ulcerative colitis?
Ulcerative colitis is not a fatal disease. However, it may cause serious complications if not treated on time.
Ulcerative colitis is a chronic condition that affects the large intestine. Learn about its causes, signs and symptoms, diagnosis, and treatment in this informative video.
Personal Experience: Source
StyleCraze's articles are interwoven with authentic personal narratives that provide depth and resonance to our content. Below are the sources of the personal accounts referenced in this article.
i. I’m Fricking Alive! (A Love Story)https://medium.com/@parkerhlyons13/im-fricking-alive-a-love-story-f06e0501a1c6
References
Articles on StyleCraze are backed by verified information from peer-reviewed and academic research papers, reputed organizations, research institutions, and medical associations to ensure accuracy and relevance. Read our editorial policy to learn more.
- Skin Manifestations of Inflammatory Bowel Disease
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3273725/ - Inflammatory Bowel Disease in Primary Immunodeficiencies
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6953999/ - New Research in Ulcerative Colitis
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2886447/ - Frequency and risk factors for extraintestinal manifestations in the Swiss inflammatory bowel disease cohort
https://www.ncbi.nlm.nih.gov/pubmed/20808297 - Hemorrhoids and anal fissures in inflammatory bowel disease
https://pubmed.ncbi.nlm.nih.gov/26446683/ - Psoriasis and Inflammatory Bowel Disease: Two Sides of the Same Coin?
https://academic.oup.com/ecco-jcc/article/9/9/697/346871 - Further evidence for an association between psoriasis, Crohn’s disease and ulcerative colitis
https://www.ncbi.nlm.nih.gov/pubmed/7066192 - Isotretinoin Use and the Risk of Inflammatory Bowel Disease: A Case Control Study
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3073620/ - Scientists Implicate Gene in Vitiligo and Other Autoimmune Diseases
https://www.nih.gov/news-events/news-releases/scientists-implicate-gene-vitiligo-other-autoimmune-diseases - Ulcerative colitis and Sweets syndrome: A case report and review of the literature
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2662205/ - Sweets syndrome complicating ulcerative colitis: a rare association
https://casereports.bmj.com/content/2016/bcr-2015-212990.full - Bowel-associated dermatosis-arthritis syndrome (BADAS) in a pediatric patient
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4949491/ - [Bowel-associated dermatosis-arthritis syndrome during ulcerative colitis: A rare extra-intestinal sign of inflammatory bowel disease]
https://www.ncbi.nlm.nih.gov/pubmed/26988382
Read full bio of Dr. Kendall R. Roehl
Read full bio of Ramona Sinha
Read full bio of Eshna Das
Read full bio of Shiboli Chakraborti

























Community Experiences
Join the conversation and become a part of our empowering community! Share your stories, experiences, and insights to connect with other beauty, lifestyle, and health enthusiasts.